- Speak to Breast Cancer Now’s expert nurses now by calling our free and confidential Helpline on 0808 800 6000 or visit forum.breastcancernow.org

21.04.2026
Help others understand health advice and receive a £25 voucher
Getting the right care, at the right time and in the right place is important for everyone. For children and young people, however, delays can have especially significant and lasting consequences. Some treatments and interventions are less effective if not administered at a specific age or developmental stage – and the opportunity to intervene can be missed completely if the wait for diagnosis is too long.
Many children and young people are not currently getting the support they need. This year’s State of Care report highlights this as a risk not just for today, but for the future. Children who do not receive the care they need today are at increased risk of becoming adults with long-term mental or physical illnesses, which could affect their quality of life and their ability to contribute to society tomorrow.
More broadly, timely access to good care continues to be a struggle for many, and inequalities in care persist. And issues getting access to services are often exacerbated by deprivation; in 2023/24, attendance rates for urgent and emergency care for people living in the most deprived areas of England were nearly double those for people in the least deprived areas.
Analysis conducted for CQC showed that for people attending for mental health reasons, the difference was over three times higher for those in the most deprived areas.
The safety and quality of some services is not good enough. CQC’s review of maternity services shows that women and babies are still not receiving the high-quality maternity care they deserve, and women from Black and ethnic minority backgrounds continue to be more at risk of experiencing poor maternity care and outcomes.
Mental health services are also a cause for serious concern. Lack of resources, ageing estates and poorly designed facilities are affecting the safety of inpatient wards. CQC’s special review of the care provided by Nottinghamshire Healthcare NHS Foundation Trust also identified wider concerns around community mental health services, leading to recommendations to improve oversight and treatment of people with serious mental health issues.
CQC has particular concerns about children and young people’s mental health services, where demand continues to rise. In 2023, 1 in 5 children and young people between the ages of 8 and 25 were estimated to have a mental health disorder. While the mental health workforce has grown, problems with staffing and skill mix remain. Across the country, services are facing challenges in recruiting staff including nurses, psychologists, occupational therapists, and consultant psychiatrists – all of which are having an impact on capacity, and therefore on the availability and regularity of appointments.
Mental health difficulties experienced as an adult often begin in childhood or young adulthood. Early intervention increases the prospects of good mental health in later life – but delayed or inadequate intervention decreases these chances.
CQC commissioned work to gain further insight into the experiences of children and young people when using mental health services. From this, one young person described the consequences of what they felt to be inadequate support from community services, leading to long-term hospitalisation:
“I didn’t know what to do because I didn’t have any GCSEs and I thought no one’s gonna want to give me a job and I’m not gonna be able to go to college…I wasn’t a normal person of my age because I was in hospital and I missed out on all the things”.
Conversely, a young person who had a positive experience reflected: “I do still think back on my time at CAMHS and I was like, if I didn’t [get that support], I would be in such a different place today… I got very lucky.”
Further research commissioned by CQC into attendances at urgent and emergency care settings by people with a mental health issue found that those aged 18 to 21 consistently have the highest rates of presentation for mental health issues at both emergency departments and urgent care centres. Not getting the right help at the right time can lead to people’s symptoms to deteriorate and they can then end up in crisis and/or inappropriate environments, such as urgent and emergency care.
CQC’s inspections of urgent and emergency care services found issues around triage and patient flow that affect care for all patients but identified specific issues around care for deteriorating children. Low numbers of children’s nurses and gaps in staff training in safeguarding and recognising sepsis meant that in some services, there was a risk that a deteriorating child might not be identified quickly, with patients at risk of sepsis not being assessed and treated promptly. Actively involving parents in their child’s care decisions and addressing their concerns promptly is critical to safety.
Last year’s State of Care warned about movement to a two-tier healthcare system – where those who can afford to pay for treatment do so and those who can’t face longer waits and reduced access. This remains a concern, starkly illustrated in dental care. CQC conducted a dental access survey of 1,000 people earlier this year, which found that people relied more on private care where NHS activity is lowest, and that access issues had a clear impact on children and young people.
Parents said they felt pressured to go private and found it difficult to get appointments, even in emergencies, and that children were left in pain while waiting for an emergency appointment. It is notable that the tooth extraction rate related to decay is nearly 3 and a half times higher for children and young people in the most deprived communities, compared with the most affluent.
The report also highlights concerns about care for autistic people and people with a learning disability – both the quality of care and access to it. The waiting time to begin assessment for a possible autism diagnosis is far too long, with average waiting times even longer for children and young people – 356 days in April 2024 compared with 238 days for adults. An autism diagnosis can be vital to getting the right help and support and can make a critical difference for children who are struggling at school.
In inspections of providers, CQC has seen examples where specialist services for children and families with complex needs were pivotal in leading multi-agency working and sharing learning. A limited review of integrated care system (ICS) plans, undertaken before the pause in CQC’s assessments of ICSs also saw some early positive signs, including transformation plans for children and young people’s services. Some ICSs have children and young people scrutiny boards to provide governance and monitor planned implementation.
Waiting times for services remain a problem within ICSs, and the main challenge is demand versus supply – a significant increase in requests at the same time as workforce shortages. There was variation between some published ICS plans or a lack of clarity about their intended outcomes. But some ICSs had examples of action already taken – for example, one described virtual wards that had supported more than 1,150 children.
However, a greater focus on children and young people’s services at both a national and local level is needed. This should include consistent funding targeted to areas of early intervention, better understanding by systems of the gaps in provision of care and treatment for their population to ensure that local areas can meet the needs of their children, improved management of demand and communication with children and their families.

Ian Dilks, Chair of CQC, said: “This year’s State of Care describes issues with access to and quality of care and the impact on people who use health and care services – with particular focus on the many children and young people who are not getting the care they need when they need it.
“While some children are receiving timely, appropriate care, we know that there are more who don’t, with potential long-term repercussions for their mental and physical health. Action now – targeted funding for early intervention, better understanding of local need and improved management of demand, and genuine two-way communication with children and families – will help to ensure a healthier population tomorrow.
“The health and wellbeing of a nation’s children has been described as the best predictor of its future prosperity; failing to ensure good, safe care for our children today also risks failing their future.”
James Bullion, Interim Chief Executive of CQC, added: “We have consistently highlighted the fragility of the adult social care sector – and the situation remains precarious.
“The number of new requests for local authority adult social care support that resulted in no service being provided has increased by over quarter over the last 5 years. And in April this year, waits for care home beds and home-based care accounted for almost half of delays in discharging patients who’d been in hospital for more than 14 days. Nearly 4,000 people are delayed on an average day – that’s 50 double-decker buses full.
“While vacancies in adult social care have dropped slightly, the average staff vacancy rate in social care is still nearly three times higher than in the national workforce – and care workers, despite the crucial job they do, remain among the lowest paid members of society.
‘Some providers are struggling to provide good, safe care – but there are also many outstanding adult social care providers who put the people they care for at the centre of their decision making, as the case studies included in this report demonstrate.”
Commenting on the report, Chris McCann, Healthwatch England’s Deputy Chief Executive said: “This report makes for disturbing reading and reflects what many people, especially parents and young people, are telling us about problems accessing care and the impact this can have.
“When it comes to dental care, these issues are particularly acute. Parents have told us that their school-aged children have never seen an NHS dentist due to a lack of available appointments. Some are told their child can only be treated under the NHS if the parent registers as a private patient. We have alerted NHS England, urging them to remind dentists that this is a breach of their contract.
“A child experiencing untreated dental problems cannot eat, sleep, or properly concentrate in class. Fundamental changes to NHS dentistry are needed urgently to improve access and prevent a new generation from living with poor oral health throughout their adulthood.
“The CQC findings also confirm experiences shared with us about other issues, such as the long waits for ADHD assessments. A problem which is highlighted by the story of one mother who sought help for her child in year three, but support didn’t start until his second year of secondary school.
“It is essential that the NHS does all it can to speed up access for patients and reduce the impact that long waits have on people’s mental and physical health.
“However, we also need long-term solutions. The government consultation on the NHS’s ten-year plan provides an opportunity to turn the corner on long waits for care. We’d urge everyone, especially parents and young people, to share their views and help shape the healthcare system for the future.”
Read the full report here.
Healthwatch England response : https://www.healthwatch.co.uk/response/2024-10-25/our-response-state-care-report
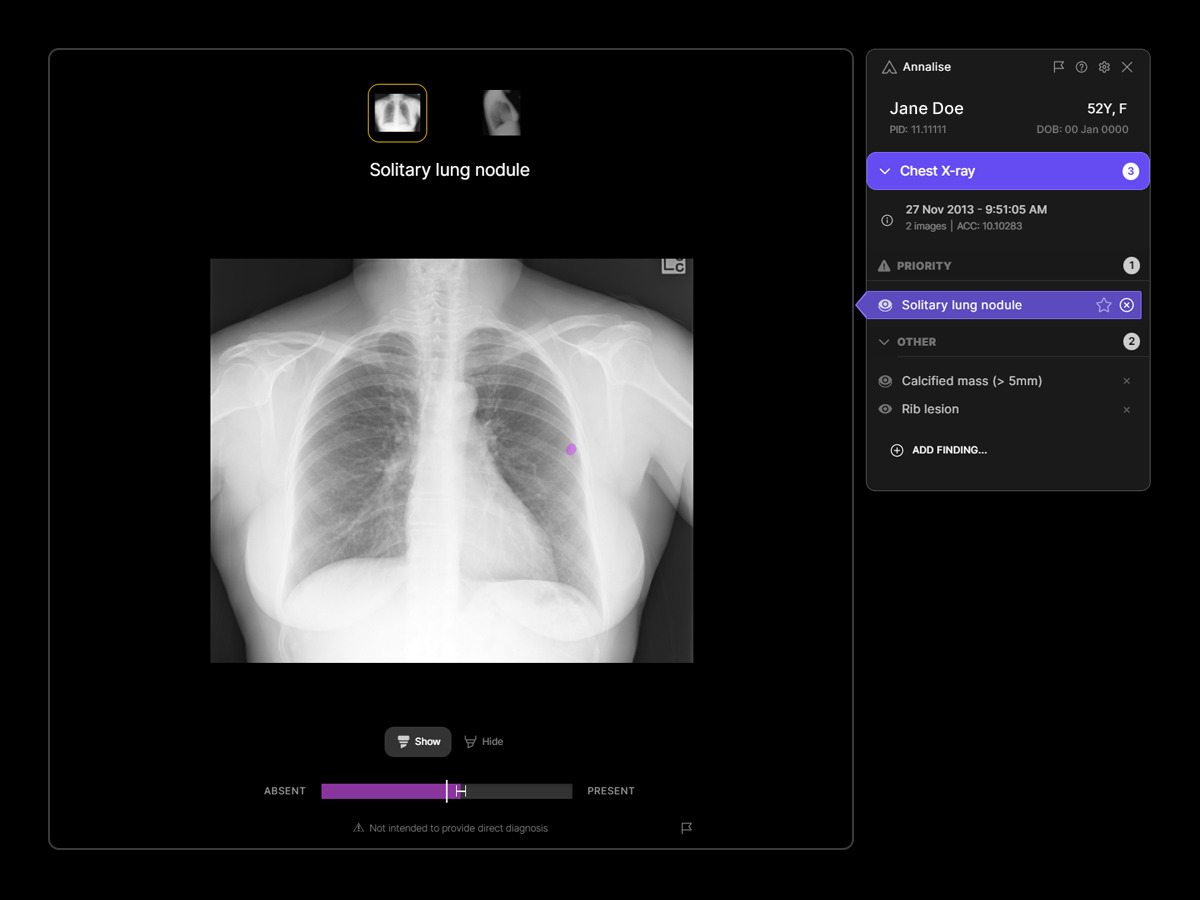
The AI technology serves as a vital second pair of eyes for clinicians, capable of prioritising cases where X-rays reveal suspicious findings that could indicate lung cancer. It has demonstrated a remarkable 45% improvement in diagnostic accuracy and a 12% boost in diagnostic efficiency.
The collaboration with Annalise.ai was made possible by a successful funding bid through the region’s Imaging Network, backed by the Provider Collaborative, which unites all NHS Foundation Trusts.
The bid gained support from the Northern Cancer Alliance and successfully secured funding from NHS England’s AI Diagnostic Fund (AIDF), which allocates £21m to provide 12 imaging networks across 65 NHS trusts in England.
Lung cancer is the leading cause of cancer death in the North East and North Cumbria.
It also has the highest incidence in England, with 117 people per every 100,000 developing the disease, compared to 88.5 people per 100,000 in London.
Six in 10 people will survive more than five years if lung cancer is diagnosed at the earlier stages, but this falls to just one in 10 for those diagnosed at the latest stage.
The disease has many causes, but a significant aspect is the higher smoking rates across generations in our region compared to the national average. The North East and North Cumbria are home to some of the most disadvantaged communities, where residents already contend with health inequalities.
The rollout of AI technology has the potential to save lives across the North East and North Cumbria, bringing hope to many individuals in their battle against cancer and strengthening our regional fight against the disease
Consultant Radiologist at South Tyneside and Sunderland NHS Foundation Trust, Dr Peter Hewitt said: “By using the AI tool, it will interpret chest X- rays within a minute of them being taken and it will put patients with suspected cancers at the top of the list for reporting.
“It will improve the accuracy and speed of reporting, acting as a second pair of eyes and will pick up anything subtle.”
Ken Bremner MBE, Chair of the North East and North Cumbria Provider Collaborative and Senior Responsible Officer for the region’s imaging network, is also Chief Executive of South Tyneside and Sunderland NHS Foundation Trust.
He said: “The arrival of this technology for the region’s NHS is a very welcome addition to our fight against lung cancer and the terrible impact it has on our region’s communities. By using the AI tool, we will be able to improve the time it takes for treatment to begin for anyone who receives a lung cancer diagnosis. It will help us to save people’s lives and, importantly, catch more cases quickly.
“The earlier we can start treatment for lung cancer the better – this will go some way to make that difficult time following a diagnosis easier for patients as they start their treatment journey.”
In 2022, mental health was the fifth most common reason given for sickness absence, accounting for 7.9% of occurrences – 15% of UK workers are estimated to have an existing mental health condition.
Mental ill health is now the most common cause of work-limiting conditions among those aged 44 years and younger.
Over the past decade, the number of workers aged 16–34 years who reported that their mental health limits the type or amount of work they can do has more than quadrupled.
Working conditions and environment can also have a significant impact on mental health. In 2022/23, there were an estimated 875,000 workers suffering from work-related stress, depression or anxiety, resulting in 17.1m working days lost.
Poor mental wellbeing costs employers in the UK an estimated £42bn to £45bn annually through presenteeism, sickness absence and staff turnover.
Recent research finds that, on average, there is a positive return on investment of around £5 for every £1 invested in mental health interventions in the workplace.
Last year there were over 7,000 events across the UK on World Mental Health Day, with over 260,000 people having conversations about mental health across their workplaces, schools, homes or the community.
The World Federation of Mental Health said: “By addressing workplace burnout on this World Mental Health Day, we can create a more productive, engaged, and fulfilled workforce.
“A mentally healthy workplace is a thriving workplace. Let’s work together to combat poor mental health and burnout and foster environments where everyone can flourish.”
This year’s theme for World Mental Health Day set by the World Federation of Mental Health is workplace mental health. It highlights the importance of addressing mental health and wellbeing in the workplace, for the benefit of people, organisations, and communities.
The Mental Health Foundation is offering a course where you can learn how to build personal strategies to improve your own mental health and well-being at work as well as supporting others.
The course could be useful if you are working in HR, a manager seeking guidance or a team member wanting to improve your workplace culture. Find out more here.
Find out more about local NHS mental health services here.
Most cancers are diagnosed in patients who have been seen by a GP and referred to hospital for investigation. However, some patients present as an emergency with “alarm” symptoms and are found to have cancer.
Those who present as an emergency often have advanced cancer and have fewer treatment options and worse outcomes than people who are diagnosed with cancer through non-emergency routes. Understanding more about the problem is expected to be an important step towards developing solutions.
The planned study will use interviews with patients and health practitioners to learn about the experiences of people who were diagnosed with cancer as an emergency. This might include learning about what led to a person presenting as an emergency as well as their experiences of that care and their treatment afterwards.
What input are the researchers looking for?
The study is at an early stage of planning and the research team would like to talk to people affected by cancer – with and without experience of emergency presentation – to hear about their experiences and their opinions about the planned study. This will help them to ensure the study will ask useful questions and include the right participants.
As the project progresses, the research team would like input from people to read and comment on study documents such as participant information sheets to make sure the language is appropriate, sensitive, and easy to understand.
Ultimately, they might ask for input to discuss the results of the study and possible next steps.
What would participants be asked to do?
Initially you would be asked to take part in a discussion with one of the researchers, either on your own or as part of a group. This would be online using Zoom or Teams. Later, if you were willing, you might be sent electronic copies of documents to look at and comment on, and/or be invited to a look at the results and discuss next steps.
If you would rather not get involved in the later steps (reviewing documents and results), it’s fine just to take part in the in the first discussion.
If you would rather not talk to the researchers but do have views or experiences you would like to share, you can also email them.
What should I do if I am interested in taking part?
If you are interested in providing input or would like more information, email Adam Biran (one of the researchers at Newcastle University) at Adam.Biran@Newcastle.ac.uk.
Its Walk of Light will be held as part of the week, which runs from Wednesday October 9 to Tuesday October 15.
The procession will gather at the foot of Penshaw Monument at 4.45pm on Monday October 14 for a 5pm start. The event, which is now in its third year, is expected to last around 90 minutes.
Charlotte Mutton is a Specialist Bereavement Lead Midwife, Subsequent Pregnancy Midwife, Pregnancy Loss Bereavement Counsellor and a Bereavement Trainer and Educator at the Trust.
She said: “We’re hosting this walk so we can come together to reflect upon and remember all of the babies who are sadly no longer with us. We know people can find it helpful to be together and this is also a time where they can have a moment to themselves in that shared moment.
“We’re inviting people to bring something with them to light their way to the top of the monument. We’ll also have a small number of lanterns available to use too.
“The walk to the top of the monument will be slow in pace. There will be music and readings as part of a reflection service at the summit and a few moments of pause to remember all babies and children who are no longer with us.
“We’ll then head back to the bottom of the monument, again without any rush to give people time to think or chat to each other. At the bottom of the hill, anyone taking part will have the chance to write their loved one’s name on a heart to hang on our memory tree.”
Christie Woods, a Bereavement Support Worker at the Trust, has played a vital role in organising the upcoming Walk of Light event as part of the Forever Cherished team.
Charlotte would like to thank Christie Wood and Jamie Renilson for their support within the services and in running the event.
There will be refreshments available at the event and the team will also hold a collection to support its Forever Cherished fund.
More details about the support available to those who have faced a loss through pregnancy can visit the Trust’s Maternity Bereavement Service page on its website: https://www.stsft.nhs.uk/services/maternity-new/maternal-mental-health-birth-reflection-and-bereavement-services/bereavement-services
Photo: Charlotte Mutton left specialist bereavement lead midwife and Jamie Renilson midwife right
The research and support charity is calling on all women to ‘get to know their normal’.
With one in ten (10%) women in the UK reporting to have never checked their breasts – which varies region to region, including increasing to 16% for women living in London – and with 13% only checking once a year or less, the charity is urging women to prioritise regular breast checking and familiarise themselves with the signs and symptoms of the disease, to help them spot any new or unusual breast changes, so they can get them checked out by a GP.
According to the YouGov findings, of the women who do check their breasts regularly for possible signs and symptoms of breast cancer, almost a third (31%) don’t feel confident that they would notice a breast change. Furthermore, only 52% of women said they would inform their GP in the first instance, if they noticed a new or unusual change in their breast(s), while 43% of women would want to seek advice, support or reassurance from someone else first.
This is cause for deep concern given around two-thirds of breast cancers in England are found when women detect a new or unusual breast change and get this checked out by a GP***, and the earlier breast cancer is diagnosed, the better the chance of successful treatment, and lives potentially being saved from this devastating disease.
When asked what stops or prevents women**** from regular breast checking, multiple barriers were revealed, including: forgetting to check (48%), not being in the habit of checking their breasts (36%), lacking confidence in checking their breasts (16%) and not knowing how to check their breasts (13%).
Manveet Basra, associate director, public health, inclusion and awareness, at Breast Cancer Now, said: “It’s deeply concerning that over two in five women in the UK aren’t regularly checking their breasts, and that only half of UK women (52%) are reporting a possible sign or symptom of breast cancer to a GP in the first instance.
“It’s clear more needs to be done to educate and support women to ‘know their normal’ and Breast Cancer Awareness Month presents a vital moment to spread these important breast health awareness messages.
“At Breast Cancer Now, we want every woman to know the importance of regular breast checking, and the many different signs and symptoms of breast cancer, so they feel empowered to regularly check their breasts, and get any new or unusual breast changes checked by a GP, along with attending NHS breast screening when invited, and breast checking in between their screening appointments.
“This is so vital when around two thirds of breast cancers in England are found when women detect anew or unusual breast change and get this checked out by a GP, and the earlier breast cancer is diagnosed, the better the chance of successful treatment, and lives potentially being saved from breast cancer.
“With the most notable barrier to women regularly breast checking being that they forget, we’re reminding women to get it back on their agenda. Checking your breasts only takes a few minutes and there’s no right way to check, as long as you’re doing it regularly.
“This could be as part of your self-care routine while getting dressed, showering or applying moisturiser. It’s important to check your whole breast area, your armpits and up to your collarbone (upper chest) for changes. At Breast Cancer Now, we say, it’s as simple as TLC: Touch, Look, Check.”
Breast cancer can cause a number of signs and symptoms which include:
On its own, pain in your breasts is not usually a sign of breast cancer, but look out for pain in your breast or armpit that’s there all or almost all the time.
Although it is rare, men can get breast cancer and the most common symptom of breast cancer in men is a lump in the chest area.
Visit breastcancernow.org/checking for more information on the signs and symptoms of breast cancer. If you’re worried about breast cancer or have a question about breast health, Breast Cancer Now is there to support you every step of the way.

The most common cancer globally with around 2.3m new cases every year, breast cancer represents one in eight cancer cases in both sexes and a quarter of all cancers in women.
With one in six cancer deaths in women worldwide, breast cancer is also the leading cause of cancer deaths among women globally.
October is Breast Cancer Awareness Month, an annual campaign to highlight ways to minimise the risk of developing the disease and to spot any signs you could have contracted it.
About one in four breast cancers can be prevented by modifying risk factors and adopting healthier lifestyle choices. The most important lifestyle choices to consider are to exercise regularly, to maintain a healthy weight and to avoid alcohol consumption. Recent studies have shown that maintaining a balanced diet and body weight can affect breast cancer risks for women 10, 20 or even 30 years later.
Healthy lifestyle choices are important but not enough alone. We must regularly look out for any breast abnormalities and seek medical advice with any concerns. This is known as breast awareness. Some women prefer to perform self-examinations. This can help. But the most important action is to be routinely monitoring our breast for any abnormality and reporting any concerns to your health care provider.
Breast cancer can affect anyone, so it’s important to check yourself regularly and get to know what’s normal for you. If you’re wondering how to be more breast aware, it’s as simple as TLC: Touch, Look, Check.
Could you help us spread the word this October? We want more people to start checking their breasts regularly. Talking to your friends, sharing things on social media or telling your colleagues about it at work – it all helps.
Breast cancer isn’t always easy to talk about. But Breast Cancer Now is listening. The Big Breast Cancer Survey is all about understanding your experience better. The charity wants to get an honest, unvarnished picture of the realities of breast cancer right now.
Breast Cancer Now is creating its next strategy – the plan it will use to guide its work over the coming years. And BCN wants the experiences of people affected by breast cancer to be at the heart of it.
This is your chance to have your voice heard. The more BCN knows, the more it can do to make sure everyone affected by breast cancer lives and is supported to live well.

Wear it pink is back for Breast Cancer Awareness Month, and Breast Cancer Now would love for you to take part!
You’d be joining thousands of people across the UK who’ll be wearing pink on Friday October 18 – at work, at school or in their community. However you wear it pink, every penny you raise will make a difference.
All you need to do to get started is order your free fundraising pack today. It includes fantastic resources, including decorations, tips and ideas as well as a donation box.
And if you need any help, just email wearitpink@breastcancernow.org!
https://breastcancernow.org/wear-it-pink/sign-up-for-wear-it-pink
* Regularly checking your breasts refers to checking at least once a week, once a month or at least once every 6 weeks. All figures, unless otherwise stated, are from YouGov Plc. Total sample size was 2,137 females. Fieldwork was undertaken between 10-12 September 2024. The survey was carried out online. The figures have been weighted and are representative of all GB females (aged 18+).
Latest news
Quick online NHS services